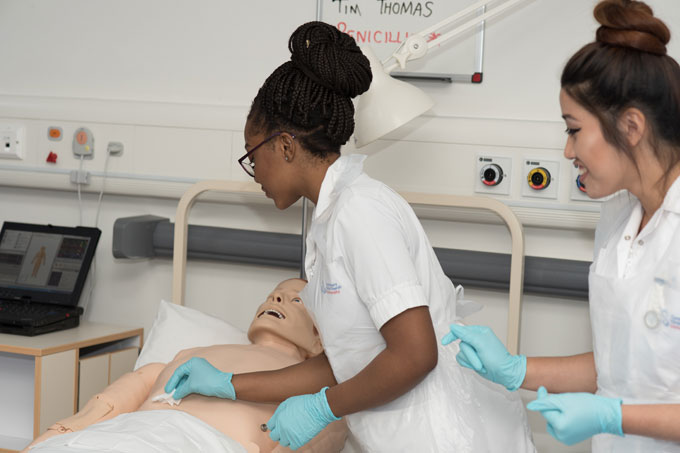
Professor Paula Kersten responds to a recent report highlighting a national increase in applications to study for a Nursing degree.
The publication of the UCAS report last week, Next Steps: Who are the ‘future nurses‘, in collaboration with Health Education England (HEE), brought welcome positive news. It reported a record number of 18-year-olds applied to study nursing in England in 2021, with the COVID pandemic playing a significant factor in their decision.
An increased interest in the nursing profession is a real positive, and a good problem to have. However, growth in nurse education is complex, with many interconnected challenges which impact on our ability to grow the workforce.
Despite a record rise in applications nationally, we are only now returning to pre-2017 levels; the year when nursing bursaries were abolished, and when we saw an immediate drop in applications. This drop was in line with sector expectations and was greatest in mature applicants (which has not yet returned to pre-2017 levels).
To ensure continued growth our students need non-means tested funding support for living costs. The recently introduced training grant of £5,000 per year, plus additional allowances for some students, helps but they are not sufficient to support with total living costs. Studying for a Nursing degree is a full-time course, and many students are not able to work alongside their study.
One of the main reasons that impedes growth in nursing student numbers is placement capacity. The NHS has been under resourced for many years. Consequently, we have insufficient placements, despite NHS Trusts and education sector working collaboratively to grow capacity.
We have been able to grow our placement numbers by thinking innovatively and using new placement models. For example, through our hub and spoke models for placements we ensure our students are placed with all the specialist nursing areas in the region. We are also providing virtual, leadership and diverse placements, which generates capacity for growth.
Nursing students complete 2,300 hours on placement as part of their degree. This is an EU Directive. Following Brexit there is an opportunity for the Nursing and Midwifery Council (NMC) to reduce these hours, an argument that has been made by Universities, the Council of Deans of Health and other lobby groups.
Indeed, there is no evidence that underpins the requirement of 2,300 hours. In many countries the practice hours requirements are much less. In Australia only 800 hours are required.
The NMC has recently allowed greater flexibility for universities by increasing the simulation hours from 300 to 600, building on our work during the pandemic, this requires further investments.
Reducing placement requirements and simulation are just two examples of achieving growth. We also need to support the health and social care sector with workforce retention and return to practice, enabling staff to work in well resourced services, with support for health and wellbeing and career development. As a university we are working in close partnership with our health and social care partners in all these areas.
People choose to work for the NHS because they want to give the best care they can. However, growth can only be achieved if we tackle all areas such as those discussed here. It is not as simple as offering more places to more applicants.
Professor Paula Kersten is Pro Vice-Chancellor and Dean of the Faculty or Medicine, Health and Social Care.
 Expert comment
Expert comment Jeanette Earl
Jeanette Earl 3318
3318